- C-BLOCK, FLAT NO, RAJAGIRI VALLEY P O, CN-3, Kalangad Rd, Kakkanad, Kerala 682039
- felix@insurancesuperhub.in

Having health insurance provides a financial safety net during medical emergencies. But simply owning a policy isn’t enough — it’s equally important to understand how to access your benefits at the time of hospitalization.
What’s the difference between a cashless claim and a reimbursement claim?
Both serve the same purpose — helping you recover medical expenses — but the process, timelines, and convenience levels differ.
Knowing how each works will help you make informed decisions during treatment.
Definition: In a cashless claim, the insurance company directly settles the hospitalization expenses with the hospital. You don’t need to pay from your own pocket upfront, except for expenses not covered by the policy (like food, toiletries, etc.).
Note: Any non-covered expenses or deductions are paid by you directly to the hospital (if Safeguard+ Add-On is not opted.)
Definition: In a reimbursement claim, the policyholder pays all medical expenses at the time of hospitalization. After discharge, they submit the required documents to the insurer, who reimburses the eligible expenses as per policy terms.
✅ Freedom to choose any hospital or doctor
✅ Useful in emergencies where network hospitals aren’t accessible
✅ Policy benefits remain intact even without cashless availability
| Aspect | Cashless Claim | Reimbursement Claim |
|---|---|---|
| Hospital Type | Network hospitals only | Any hospital |
| Payment | Insurer pays directly to hospital | Insured pays first, then claims |
| Documentation | Minimal (handled by hospital/TPA) | Insured collects and submits |
| Approval Process | Pre-authorization before treatment | Post-treatment document review |
| Timeline | During hospitalization (quick) | After discharge (7–30 days avg.) |
| Convenience | High | Moderate |
| Out-of-pocket expenses | Minimal (non-medical only) | High upfront, reimbursed later |
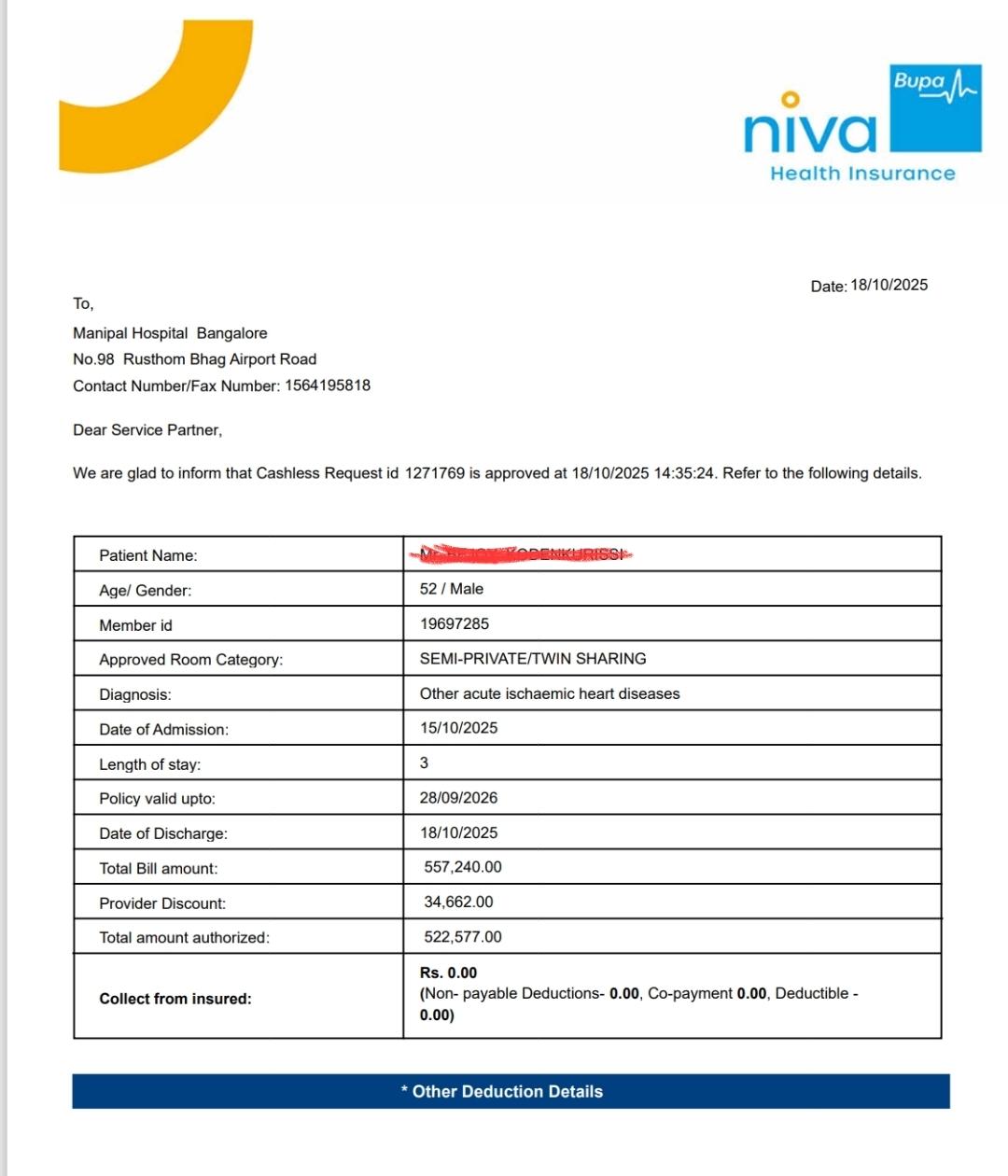
If Safeguard+ Add-On is Opted, then all non-medical/consumable items listed in Annexure list 1-4 will be covered. There won' be any out of pocket expenses. Pls refer the final discharge confirmation received from company👇
| Scenario | Recommended Claim Type |
|---|---|
| Planned treatment at a network hospital | Cashless |
| Emergency treatment at a network hospital | Cashless (if possible) |
| Treatment at a hospital outside the network | Reimbursement |
| No time for pre-authorization | Reimbursement |
❌ Myth 1: Cashless means no payments at all.
✅ Reality: Some expenses like consumables, registration, and non-medical items may still need to be paid by the patient.
❌ Myth 2: Reimbursement claims always take months.
✅ Reality: Most insurers process them within 7-30 working days if documents are complete.
❌ Myth 3: Reimbursement is a backup; cashless is always better.
✅ Reality: Both serve valid needs. Reimbursement provides flexibility when cashless is not feasible.
A well-informed customer experiences fewer hassles and greater satisfaction during claims.
Both cashless and reimbursement claims exist to ensure that you’re financially protected during medical emergencies. The main difference lies in the process and convenience, not the coverage.
Understanding these options in advance helps you choose the most suitable path during treatment and reduces stress during already difficult times.